Cardiac arrest patients who are treated with adrenaline are significantly more likely to have severe brain damage if they survive, a new study has found.
Adrenaline is routinely used as a last resort when other treatments fail.
A study of 8,000 patients found that while it slightly increased the chances of survival, patients who had adrenaline were much more likely to end up severely disabled.
Policymakers said they would look at the study’s findings in detail.
Each year about 30,000 people in the UK have a cardiac arrest – where the heart suddenly stops pumping blood around the body.
It is more dangerous than a heart attack, with less than one in 10 cardiac arrest patients surviving.
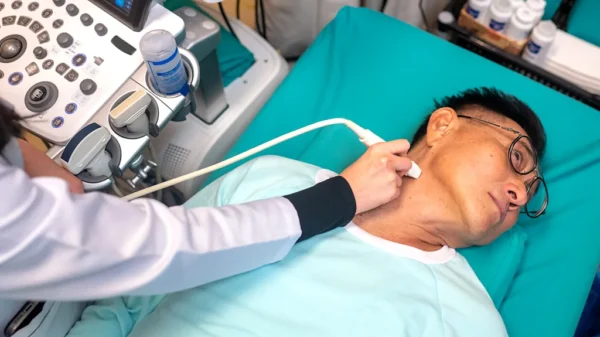
Treating the condition quickly with cardiopulmonary resuscitation (CPR) and defibrillation offers the best chances of survival.
When these fail, current guidance recommends injections of adrenaline in order to try to restore a heartbeat – a practice that has been in place for nearly 60 years.
But increasingly there has been evidence to suggest the treatment may result in worse long-term survival rates and greater brain damage in patients.
For this new trial, cardiac arrest patients from England and Wales were given either an injection of adrenaline or a saltwater solution (a dummy treatment) by paramedics, who did not know which they were giving.
The three-year study found that of the 4,012 patients given adrenaline, 130 (3.2%) were alive 30 days after treatment compared with 94 (2.4%) of the 3,995 patients who had been given the saltwater solution.
However, in the adrenaline group 39 of those who went on to be discharged from hospital had severe brain damage compared with 16 who had received a placebo.
This meant that 87 people from the adrenaline group (2.2%) survived with a “favourable neurological outcome” (defined as anything from a moderate disability to no disability at all) compared to 74 (1.9%) in the placebo group – a difference researchers said was not statistically significant.
 Treating cardiac arrest quickly with CPR and defibrillation offers the best chances of survival
Treating cardiac arrest quickly with CPR and defibrillation offers the best chances of survival
Prof Gavin Perkins, one of the paper’s authors, from Warwick Medical School, at the University of Warwick, said: “Patients may be less willing to accept burdensome treatments if the chances of recovery are small or the risk of survival with severe brain damage is high.
“The findings of this trial will require careful consideration by the wider community and those responsible for clinical practice guidelines for cardiac arrest.”
Authors of the study, published in the New England Journal of Medicine, said it was not yet fully understood why those who received adrenaline had more brain damage.
One of their theories is that although adrenaline increases blood flow in large blood vessels, it impairs it in very small vessels, which may worsen brain damage caused by a cardiac arrest.
Alternatively, it may be the case that adrenaline led to more people with severe brain damage surviving.
Dr David Nunan, senior researcher at the Centre for Evidence-Based Medicine at the University of Oxford, said the “landmark trial” would change the way people are treated.
But Prof Kevin McConway, emeritus professor of applied statistics at The Open University, said deciding whether to change the guidelines would not be an easy decision to make.
“Is it worth being treated with adrenaline if it slightly increases one’s chances of surviving, even if one might only survive in a state of considerable disability? I think that’s a bit difficult to say, overall.”
Ethical approval
Researchers acknowledged their study raised “significant ethical issues”.
In February, the family of a woman who died from a cardiac arrest, Trudy Jones, from Wrexham, said they only found out she had been involved in the study at the inquest into her death.
Researchers said the urgency of cardiac arrest treatment meant it had been impossible to seek the consent of patients to take part in the trial before they had been treated, as would usually be the case.
Instead, families were contacted afterwards for consent if the patient survived.
The researchers, who gained ethical approval for the study, added that a public awareness campaign about the trial had run before it had started, offering people the chance to opt out.
The Resuscitation Council, which helps write the guidelines for resuscitation used by health professionals, said it would look at the study in detail, as it expected it to inform future UK guidelines.
Source: www.bbc.com